Venous Disease develops when damaged vein walls and weakened valves disrupt normal blood circulation. The veins allow blood to flow backward and collect when muscles relax, which creates increased pressure inside the veins. This pressure buildup reduces proper blood return to the heart and leads to swelling, discomfort, and visible vein problems.
Leg veins carry deoxygenated blood from the limbs back to the heart against gravity. Venous Disease can cause leg pain when superficial vein valves fail and allow blood to flow backward. Deep vein problems may also develop in the pelvis when increased pressure affects the iliac veins, slowing or blocking blood flow from the legs.
Pelvic or iliac vein compression can lead to leg pain, swelling, discoloration, ulcerations, cellulitis, infections, and blood clot formation. A blood clot may break loose and travel to the lungs, causing a pulmonary embolism (PE). Symptoms of pulmonary embolism include shortness of breath and an increased heart rate.
Deep Vein Thrombosis (DVT) occurs when a blood clot forms in the deep venous system. Patients diagnosed with DVT face a higher risk of pulmonary embolism.
Superficial Vein Thrombosis (SVT) occurs when a clot forms in the superficial veins near the skin surface. It may cause redness and pain, but doctors typically manage it less aggressively because it carries a lower risk of pulmonary embolism than DVT.
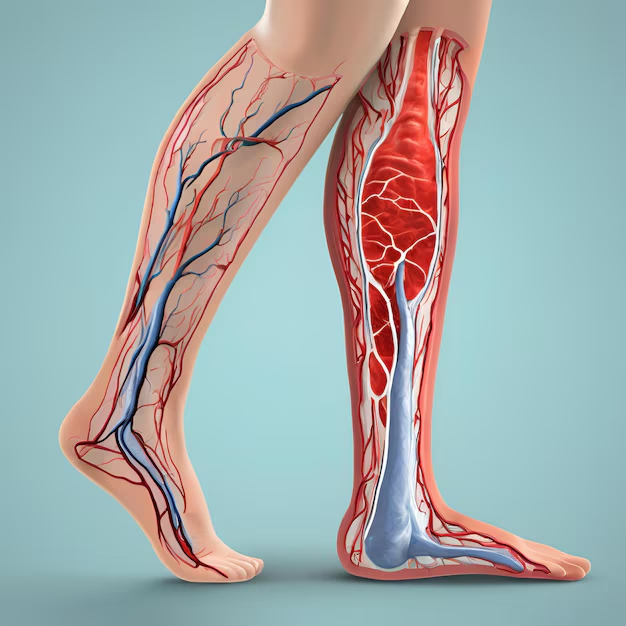
Venous Disease occurs when leg veins fail to return blood efficiently to the heart. Most patients report a heavy or aching feeling in the legs, especially after long periods of standing or sitting. Swelling in the ankles and lower legs often worsens by the end of the day and improves with rest or leg elevation.
As the condition progresses, physical changes become more visible. Varicose veins and spider veins may appear on the skin surface. The skin around the ankles may become itchy, dry, darkened, or thickened. Many patients experience burning, throbbing, or cramping pain. Elevating the legs usually reduces discomfort.
In advanced stages, Venous Disease can progress to chronic venous insufficiency and lead to slow-healing wounds or venous ulcers near the ankle. If Deep Vein Thrombosis develops, symptoms may include sudden swelling in one leg, warmth, redness, and severe pain. Seek immediate medical attention for sudden or severe symptoms.


If you experience symptoms or have risk factors for Venous Disease, schedule a consultation today. Our vascular specialists provide advanced, patient-centered care designed to improve circulation and protect your long-term vein health.
Venous Disease primarily develops when vein valves weaken or become damaged. These valves normally keep blood flowing toward the heart. When they fail, blood pools in the legs and increases pressure inside the veins.
Weak valves allow blood to flow backward and collect in the legs. This pooling increases venous pressure and contributes to swelling, varicose veins, and chronic venous insufficiency.
Blood clots block normal circulation and trigger pain, swelling, and inflammation. Without treatment, clots can permanently damage veins and increase the risk of post-thrombotic syndrome or pulmonary embolism.
Excess body weight increases pressure on leg veins and makes it harder for blood to return to the heart. Over time, this strain weakens vein walls and promotes chronic venous disease.
Several factors increase the likelihood of developing Venous Disease by affecting circulation and vein health.
A family history of varicose veins, blood clots, or chronic venous insufficiency increases genetic risk. Obesity, pregnancy, prolonged sitting, smoking, and hormone therapy also contribute. Additional risk factors include age over 60, previous vein injury, immobility, and a history of Deep Vein Thrombosis (DVT).
Chronic Venous Insufficiency (CVI) represents an advanced stage of Venous Disease. The veins lose their ability to return blood efficiently, causing persistent swelling, leg heaviness, and skin thickening. In severe cases, venous ulcers develop near the ankles and require specialized treatment to prevent infection.
Why Vascular Care Centers?
At Vascular Care Centers, we deliver comprehensive vascular care focused on accurate diagnosis and effective treatment. Our experienced vascular surgeons use advanced technology to manage Venous Disease and prevent serious complications.
Deep Vein Thrombosis (DVT) occurs when a blood clot forms in a deep vein, typically in the legs. The clot blocks blood flow and causes swelling, pain, warmth, and redness. If the clot travels to the lungs, it can cause a life-threatening pulmonary embolism. Early diagnosis and treatment reduce long-term complications.
Why Vascular Care Centers?
We combine expertise, modern technology, and compassionate care to treat Venous Disease effectively. Our goal is to relieve symptoms, restore healthy blood flow, and improve your overall quality of life.
Do not ignore leg pain, swelling, numbness, or heaviness. These symptoms may signal early Venous Disease. Adults over 50, individuals with obesity, and patients with a history of blood clots should seek evaluation even without severe symptoms.
Our specialists review your medical history and evaluate blood flow in your legs. We use diagnostic tools such as ultrasound, venogram, blood tests, and vascular imaging studies to confirm the diagnosis and determine the most effective treatment plan.
The doctor may advise you simple treatments if your symptoms are mild such as:
The doctor may advise you simple treatments if your symptoms are mild such as:
The doctor may advise you simple treatments if your symptoms are mild such as:
Your vascular specialist will evaluate circulation and recommend appropriate procedures based on the severity of Venous Disease.
Duplex vascular ultrasound uses sound waves to visualize veins and arteries and measure blood flow. This test helps detect blockages, valve dysfunction, and clot formation.
Angioplasty widens narrowed veins, and a stent keeps the vessel open to restore proper blood circulation.
Thrombolysis delivers clot-dissolving medication directly into the affected vein. Thrombectomy removes the clot to reestablish healthy blood flow.